AI Reveals How Each Country Can Boost Cancer Survival


AI has revealed why cancer survival differs so dramatically around the world, highlighting the specific health system factors that matter most in each country.
Researchers have, for the first time, applied machine learning, a form of artificial intelligence (AI), to pinpoint the factors most closely linked to cancer survival across nearly every country worldwide.
The findings appear today (January 13) in the leading cancer journal Annals of Oncology. The research goes beyond broad global trends by showing which specific policy actions or system improvements could most effectively boost cancer survival in individual countries. Through an online tool developed by the team, users can select a country and explore which elements, including national income, access to radiotherapy, and universal health coverage, are most strongly connected to cancer outcomes.
Turning Data Into Actionable Policy Guidance
Dr. Edward Christopher Dee, a resident physician in radiation oncology at Memorial Sloan Kettering (MSK) Cancer Center in New York, USA, and a co-leader of the study, emphasized the wide differences in cancer outcomes across nations. “Global cancer outcomes vary greatly, largely due to differences in national health systems. We wanted to create an actionable, data-driven framework that helps countries identify their most impactful policy levers to reduce cancer mortality and close equity gaps.”
He added that several factors repeatedly stood out. “We found that access to radiotherapy, universal health coverage and economic strength were often important levers being associated with better national cancer outcomes. However, other key factors were relevant as well.”
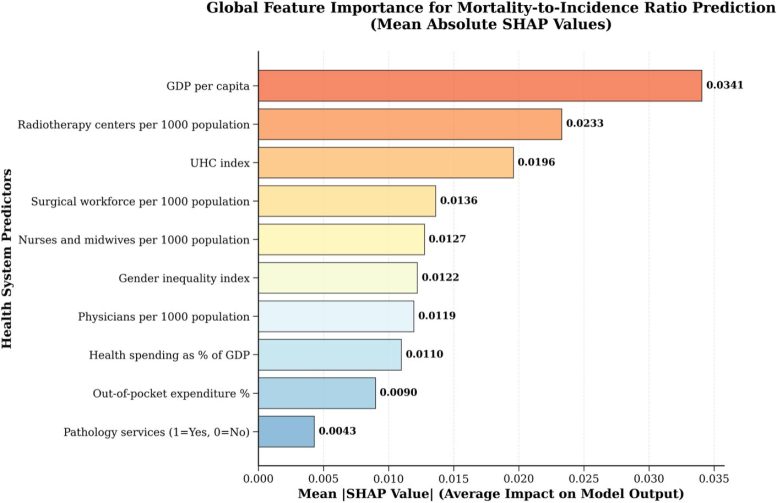
Analyzing Cancer Data From 185 Countries
To build the model, Dr. Dee and his colleagues analyzed cancer incidence and death data from the Global Cancer Observatory (GLOBOCAN 2022), covering 185 countries. They combined this with health system data from the World Health Organization, the World Bank, United Nations agencies, and the Directory of Radiotherapy Centres.
The information included health spending as a share of GDP, GDP per capita, the number of physicians, nurses, midwives, and surgical staff per 1000 people, levels of universal health coverage, access to pathology services, human development indicators, radiotherapy center availability per 1000 people, a gender inequality index, and the share of healthcare costs paid out of pocket.
Building the Machine Learning Model
The machine learning model was developed by Mr, Milit Patel, the study’s first author. He is a researcher in biochemistry, statistics and data science, healthcare reform and innovation at the University of Texas at Austin, USA, and at MSK.
Mr, Patel explained why this approach was chosen. “We chose to use machine learning models because they allow us to generate estimates – and related predictions – specific to each country. We are, of course, aware of the limitations of population level data but hope these findings can guide cancer system planning globally.”
Measuring Cancer Care Effectiveness
The model focuses on mortality-to-incidence ratios (MIR), which represent the share of cancer cases that result in death and serve as an indicator of how effective cancer care is within a country. To clarify how each factor influences the results, the researchers used a method that explains individual predictions by calculating the contribution of each variable, known as SHAP (Shapley Additive exPlanations).
According to Mr. Patel, the goal was practical impact. “Beyond simply describing disparities, our approach provides actionable, data-driven roadmaps for policymakers, showing precisely which health system investments are associated with the greatest impact for each country. As the global cancer burden grows, these insights can help nations prioritize resources and close survival gaps in the most equitable and effective way possible. International organizations, healthcare providers, and advocates may also use the web-based tool to highlight areas for investment, especially in resource-limited settings.”
Country Examples Highlight Different Priorities
The analysis reveals that the most influential factors differ by country. In Brazil, for instance, universal health coverage (UHC) shows the strongest positive association with improved mortality-to-incidence ratios. Other factors, such as pathology services and the number of nurses and midwives per 1000 people, appear to have less influence at present. Based on these findings, the researchers suggest that expanding UHC should be a top priority for Brazil.
In Poland, the availability of radiotherapy services, GDP per capita, and the UHC index have the greatest impact on cancer outcomes. This pattern suggests that recent efforts to strengthen health insurance and access to care have produced larger gains than general health spending, which shows a more modest effect.
Japan, the USA, and the UK display a different picture. In these countries, nearly all health system factors are linked to better cancer outcomes. The density of radiotherapy centers stands out most strongly in Japan, while GDP per capita has the largest impact in the USA and the UK. These results point to where policymakers may achieve the greatest benefits.
China presents a more complex mix. Higher GDP per capita, broader UHC, and greater access to radiotherapy centers contribute most to improved cancer outcomes. In contrast, out-of-pocket spending, the size of the surgical workforce per 1000 people, and health spending as a percentage of GDP are currently less effective in explaining outcome differences.
The researchers note in their paper: “High direct costs for patients remain a critical barrier to optimal cancer outcomes, even amidst national improvements in health financing and access. These findings underscore that while China’s rapid health system development is yielding important gains in cancer control, disparities in financial protection and coverage persist, warranting intensified policy focus on reducing out-of-pocket expenditures and further strengthening UHC implementation to maximize health system impact.”
Understanding the Green and Red Indicators
Mr, Patel also clarified how to interpret the green and red bars shown in the country-specific graphs. “The green bars represent factors that currently appear most strongly and positively associated with improved cancer outcomes in a given country. These are areas where continued or increased investment is most likely to result in meaningful impact.”
He cautioned against misreading the red bars. “However, the red bars do not indicate that these areas are unimportant or should be neglected. Rather, they reflect domains that, according to the model and current data, are less likely to explain the largest differences in outcomes right now. This may be due to already strong performance in these aspects, limitations of the available data, or other context-specific factors.”
He added that weaker associations should not discourage continued improvement. “Importantly, seeing a ‘red’ bar should never be interpreted as a reason to stop efforts to strengthen that pillar of cancer care – improvement in those areas can still be valuable for a country’s overall health system. Our results simply suggest that, if the goal is to maximize improvement in cancer outcomes as defined by the model, focusing first on the strongest positive (green) drivers may be the most impactful strategy.”
Strengths, Limits, and the Road Ahead
The study’s strengths include its near-global coverage, use of current international health data, country-specific policy insights rather than global averages, and the use of more transparent AI methods. At the same time, the researchers acknowledge important limitations. The analysis relies on national-level data rather than individual patient records, data quality varies widely between countries, especially in low-income regions, and national trends can mask inequalities within countries. In addition, the study cannot prove that changing a specific factor will directly cause better cancer outcomes, only that such changes are associated with improved results.
Despite these caveats, the findings offer a valuable tool for prioritization. Dr. Dee concluded: “As the global cancer burden grows, this model helps countries maximize impact with limited resources. It turns complex data into understandable, actionable advice for policymakers, making precision public health possible.”
Reference: “Machine learning reveals country-specific drivers of global cancer outcomes” by M.S. Patel et al., 13 January 2026, Annals of Oncology.
DOI: 10.1016/j.annonc.2025.11.014
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
link







